Urticaria Allergic rhinitis Mental health
Posted: 9th April 2026 | Posted by allergy
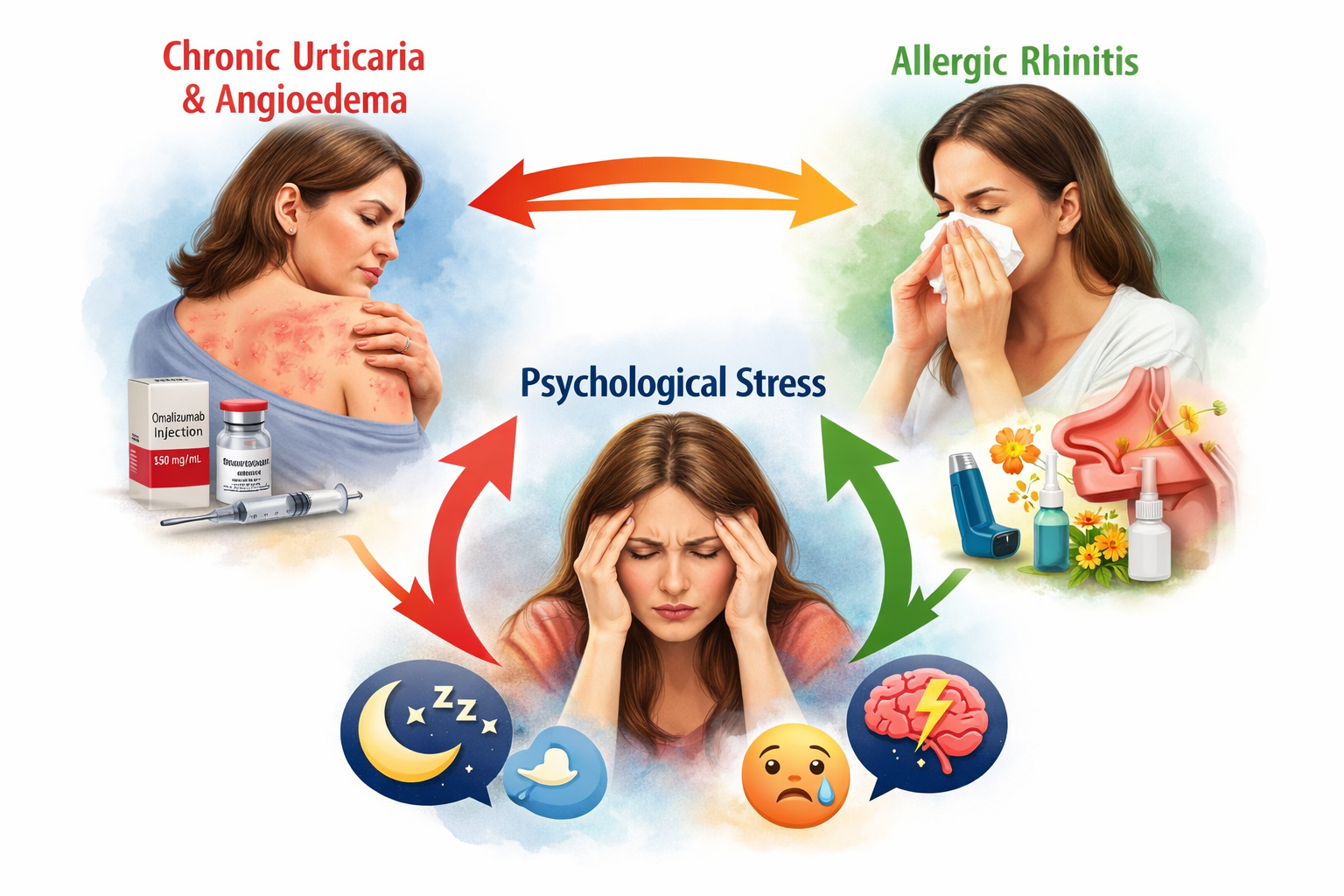
The connection between chronic urticaria, allergic rhinitis and psychological stress affecting overall wellbeing.
Why this matters for patients with allergy and urticaria
Chronic spontaneous urticaria, often called CSU, is more than a skin rash. It can disrupt sleep, affect confidence, interfere with work and family life, and create constant uncertainty because symptoms may flare without warning. When allergic rhinitis is also present, the burden can become even greater. Nasal blockage, sneezing, poor sleep and persistent irritation may add to fatigue and emotional strain.
A 2026 study explored this triad of mind, mucosa and skin and showed that psychiatric comorbidities were very common among adults with antihistamine-refractory CSU receiving omalizumab. The findings support a more integrated model of care in which allergy, skin symptoms, sleep and mental wellbeing are considered together rather than separately.
What is chronic spontaneous urticaria?
Urticaria is characterised by itchy raised wheals, angioedema, or both. When symptoms persist for more than 6 weeks, the condition is defined as chronic urticaria. If the rash and swelling occur without a clear external trigger, it is called chronic spontaneous urticaria.
Many patients improve with antihistamines, but some continue to have frequent symptoms despite treatment. In these more difficult cases, specialist assessment is important to confirm the diagnosis, identify associated conditions, assess disease activity properly and consider advanced treatment options such as omalizumab where appropriate.
– Swelling of the lips, eyelids, hands or other areas
– Symptoms lasting longer than 6 weeks
– Unpredictable flare-ups
– Sleep disturbance and reduced quality of life
What did the 2026 study find?
The study reviewed 72 adults with antihistamine-refractory CSU who received omalizumab and had a formal psychiatric evaluation at a tertiary allergy centre between 2015 and 2025. Most participants were female, with a median age of 45 years. Psychiatric diagnoses were identified in 90.3% of the cohort who underwent psychiatric assessment.
The most frequent psychiatric diagnostic group was anxiety disorders, followed by mood disorders and sleep-wake disorders. Generalised anxiety disorder was the single most common diagnosis. The authors also reported that allergic rhinitis was present in more than half of the cohort, suggesting an important upper-airway allergic burden in this patient group.
| Study finding | Result |
|---|---|
| Patients included | 72 adults with antihistamine-refractory CSU treated with omalizumab |
| Female participants | 70.8% |
| Median age | 45 years |
| Any psychiatric comorbidity | 90.3% |
| Most common psychiatric group | Anxiety disorders |
| Allergic rhinitis in the cohort | 51.4% |
Why allergic rhinitis may worsen the overall burden
Allergic rhinitis is sometimes seen as a minor condition, but persistent nasal symptoms can have a major effect on quality of life. Blocked nose, sneezing, post-nasal drip, poor sleep and daytime fatigue may all contribute to irritability, reduced concentration and lower resilience. In patients who also have chronic urticaria, this can intensify the sense of being unwell.
The authors of the study suggested that allergic rhinitis may reinforce the psychodermatological loop by adding sleep disruption and chronic upper-airway inflammation to an already stressful skin condition. This is one reason why it is important for specialist clinics to assess the whole allergic picture rather than looking at hives in isolation.
– Greater tiredness during the day
– Higher stress levels
– Lower quality of life
– A stronger perception that symptoms are difficult to control
The stress-skin connection in chronic urticaria
Patients often tell us that stress seems to aggravate their hives. This fits with what clinicians and researchers have observed for many years. Chronic urticaria can itself be stressful because flare-ups are unpredictable and visible. At the same time, stress may influence inflammatory pathways, itch perception and symptom severity, which can then further increase anxiety and distress. This creates a self-perpetuating cycle.
The 2026 paper describes this as a close interaction between psyche and skin. Biological pathways thought to be involved include stress-related neuroimmune signalling and mast cell-mediated inflammation. For patients, the important message is simple: the symptoms are real, the burden is real, and both the physical and emotional impact deserve proper attention.
This does not mean urticaria is “just stress”. Rather, it means stress, sleep problems, allergy symptoms and inflammation may all affect one another. That is why good management often requires more than a prescription alone.
Response to treatment in the study
Under omalizumab treatment, disease control improved significantly in this cohort. Median UAS7 scores fell from 42 before treatment to 7 at 24 months, while UCT scores rose from 0 to 14. These results support the role of specialist treatment in patients whose symptoms remain poorly controlled on antihistamines alone.
The authors also noted that improving urticaria control may bring psychological benefits and better emotional wellbeing. In practice, this reinforces the importance of identifying uncontrolled disease early and ensuring that patients receive an expert review rather than simply repeating ineffective treatment.
What this means for care at our ACARE and UCARE accredited centre
As an ACARE and UCARE accredited centre, we believe patients with chronic urticaria deserve expert, evidence-based and compassionate care. This includes careful diagnosis, assessment of angioedema and inducible triggers, review of coexisting allergic diseases such as allergic rhinitis and asthma, and evaluation of how symptoms are affecting sleep, mood and daily functioning.
Where appropriate, management may involve optimisation of antihistamines, consideration of advanced treatment pathways, investigation of associated conditions and practical support around trigger awareness, sleep hygiene and stress reduction. In some cases, collaboration with other professionals may be helpful so that care is truly patient-centred and holistic.
For patients, the key message is that severe hives and swelling are not only skin symptoms. They can affect confidence, sleep, relationships and quality of life. Recognising that full burden is an important step towards better outcomes.
When to seek specialist urticaria assessment
– Symptoms keep returning despite antihistamines
– You have troublesome angioedema
– Sleep is regularly disturbed by itch or nasal symptoms
– You feel that stress, anxiety or low mood are making symptoms harder to manage
– You may have both urticaria and allergic rhinitis
Book an expert review
If you are living with chronic hives, angioedema or allergic rhinitis, our specialist team can help assess the full picture and create a personalised plan. We offer consultant-led allergy care with a focus on accurate diagnosis, better symptom control and improved quality of life.
Reference
This article is based on the 2026 paper by Zeynep Yegin Katran, İsmet Bulut, Andaç Salman, Ali Baz, Galip Muzaffer Kürşat Küçükali and Özge Argın, which examined the relationship between chronic spontaneous urticaria, allergic rhinitis and psychiatric comorbidities in omalizumab-treated adults.
Please note that this blog is for general education and does not replace personalised medical advice. Diagnosis and treatment should always be based on an individual clinical assessment.
